 Image via Wikipedia
Image via Wikipedia
Definition:
Crohn’s disease (also known as regional enteritis) is a chronic, episodic, inflammatory bowel disease (IBD) and is generally classified as an autoimmune disease. Crohn’s disease can affect any part of the gastrointestinal tract from mouth to anus; as a result, the symptoms of Crohn’s disease vary among afflicted individuals. The disease is characterized by areas of inflammation with areas of normal lining between in a symptom known as skip lesions. The main gastrointestinal symptoms are abdominal pain, diarrhea (which may be bloody, though this may not be visible to the naked eye), constipation, vomiting, weight loss or weight gain. Crohn’s disease can also cause complications outside of the gastrointestinal tract such as skin rashes, arthritis, and inflammation of the eye.
The disease was independently described in 1904 by Polish surgeon Antoni Lesniowski and in 1932 by American gastroenterologist Burrill Bernard Crohn, for whom the disease was named. Crohn, along with two colleagues, described a series of patients with inflammation of the terminal ileum, the area most commonly affected by the illness. Crohn’s disease affects between 400,000 and 600,000 people in North America. Prevalence estimates for Northern Europe have ranged from 27–48 per 100,000. Crohn’s disease tends to present initially in the teens and twenties, with another peak incidence in the fifties to seventies, although the disease can occur at any age.
Although the cause of Crohn’s disease is not known, it is believed to be an autoimmune disease that is genetically linked. The highest relative risk occurs in siblings, affecting males and females equally. Smokers are three times more likely to get Crohn’s disease.
Unlike the other major types of IBD, there is no known drug based or surgical cure for Crohn’s disease. Treatment options are restricted to controlling symptoms, putting and keeping the disease in remission and preventing relapse.
CLICK & SEE THE PICTURES
The three most common sites of intestinal involvement in Crohn’s disease are ileal, ileocolic and colonic.
Symptoms:
T the symptoms of crohn’s disease vary among individuals. The disorder usually recurs at intervals throughout life. Episodes of the disease may be severe, lasting weeks or several months before settling down to periods with mild or no symptoms. The symptoms include:
· Diarrhea.
· Abdominal pain.
· fever.
· Weight loss.
· General feeling of malaise.
If the colon is affected, symptoms may also include the following:
· Diarrhea, often containing blood.
· Bloody discharge from the anus.
About 1 in 10 people also develops other disorders associated with crohn’s disease. These other conditions may occur even in mold cases of crohn’s disease and include arthritis, eye disorders, kidney disorders, gallstones, and a rash.
Causes:
The exact cause of Crohn’s disease is unknown. However, genetic and environmental factors have been invoked in the pathogenesis of the disease. Research has indicated that Crohn’s disease has a strong genetic link. The disease runs in families and those with a sibling with the disease are 30 times more likely to develop it than the normal population. Ethnic background is also a risk factor. Until very recently, whites and European Jews accounted for the vast majority of the cases in the United States, and in most industrialized countries, this demographic is still true.
Mutations in the CARD15 gene (also known as the NOD2 gene) are associated with Crohn’s disease and with susceptibility to certain phenotypes of disease location and activity. In earlier studies, only two genes were linked to Crohn’s, but scientists now believe there are over eight genes that show genetics play a crucial role in the disease.
A handful of cases of Crohn’s disease cases were reported at the turn of the 20th century, but since then, the disease has continued to increase in prevalence dramatically. Some argue that this increase has been the result of a genetic shift in the population caused by conditions favoring individuals carrying the genes linked with the disease. These conditions could be a lower infant mortality rate or better health care in the nations that have the highest incidence of disease (industrialized nations).
Others argue that Crohn’s disease is caused by a combination of environmental and genetic factors. Many environmental factors have also been hypothesized as causes or risk factors for Crohn’s disease. Proven environmental risk factors include living in an industrialized country, smoking, and living in an urban area. Diets high in sweet, fatty or refined foods may also play a role. A retrospective Japanese study found that those diagnosed with Crohn’s disease had higher intakes of sugar, fat, fish and shellfish than controls prior to diagnosis. A similar study in Israel also found higher intakes of fats (especially chemically modified fats) and sucrose, with lower intakes of fructose and fruits, water, potassium, magnesium and vitamin C in the diets of Crohn’s disease sufferers before diagnosis, and cites three large European studies in which sugar intake was significantly increased in people with Crohn’s disease compared with controls. Certain chemicals in the diet, known as microparticles, are also hypothesized as a risk factor for the disease, as well as a poor imbalance of omega-6 to healthy omega-3 fatty acids that emerging research shows helps to improve all types of inflammatory disease. The most common forms of microparticles include titanium dioxide, aluminosilicates, anatase, calcium phosphate, and soil residue. These substances are ubiquitous in processed food and most toothpastes and lip glosses. Soil residue is found on fresh fruits and vegetables unless carefully removed.
Smoking has been shown to increase the risk of the return of active disease, or “flares”. The introduction of hormonal contraception in the United States in the 1960’s is linked with a dramatic increase in the incidence rate of Crohn’s disease. Although a causal linkage has not been effectively shown, there remain fears that these drugs work on the digestive system in similar ways to smoking.
Additionally, many in the scientific community believe that early childhood exposure to illness is necessary to the creation of a proper immune system for those with the genetic susceptibility for Crohn’s Disease. Higher incidences of Crohn’s Disease are associated with cleaner living conditions. Throughout the early and mid-20th century in the United States, the disease was strongly associated with upper-class populations, and today the disease does not yet exist in the many Third World countries, despite the fact that it occurs in all races. CD is also associated with first born and single children (because they would have less exposure to childhood illness from siblings) and in populations that have low incidences of gastric cancer. Gastric cancer is most often caused by the bacterium Helicobacter pylori that flourishes in cramped and unsanitary conditions.
Abnormalities in the immune system have often been invoked as being causes of Crohn’s disease. It has been hypothesized that Crohn’s disease involves augmentation of the Th1 of cytokine response in inflammation. The most recent gene to be implicated in Crohn’s disease is ATG16L1, which may reduce the effectiveness of autophagy, and hinder the body’s ability to attack invasive bacteria.
A variety of pathogenic bacteria were initially suspected of being causative agents of Crohn’s disease. However, the current consensus is that a variety of microorganisms are simply taking advantage of their host’s weakened mucosal layer and inability to clear bacteria from the intestinal walls, both symptoms of the disease. Some studies have linked Mycobacterium avium subsp. paratuberculosis to Crohn’s disease, in part because it causes a very similar disease, Johne’s disease, in cattle. The mannose bearing antigens, mannins, from yeast may also elicit pathogenic anti saccharomyces cerevisiae antibodies. Newer studies have linked specific strains of enteroadherent E. coli to the disease but failed to find evidence of contributions by other species.
Diagnosis:
The diagnosis of Crohn’s disease can sometimes be challenging, and a number of tests are often required to assist the physician in making the diagnosis. Even with a full battery of tests it may not be possible to diagnose Crohn’s with complete certainty; a colonoscopy is approximately 70% effective in diagnosing the disease with further being less effective. Disease in the small bowel is particularly difficult to diagnose as a traditional colonoscopy only allows access to the colon and lower portions of the small intestines; recent introduction of Capsule endoscopy aid in endoscopic diagnosis.
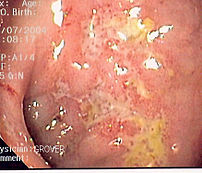
Endoscopy
A colonoscopy is the best test for making the diagnosis of Crohn’s disease as it allows direct visualization of the colon and the terminal ileum, identifying the pattern of disease involvement.
Radiologic Tests
A small bowel follow-through may suggest the diagnosis of Crohn’s disease and is useful when the disease involves only the small intestine. Because colonoscopy and gastroscopy allow direct visualization of only the terminal ileum and beginning of the duodenum, they cannot be used to evaluate the remainder of the small intestine.
CT and MRI scans are useful for evaluating the small bowel with enteroclysis protocols.They are additionally useful for looking for intra-abdominal complications of Crohn’s disease such as abscesses, small bowel obstruction, or fistulae. Magnetic resonance imaging (MRI) are another option for imaging the small bowel as well as looking for complications, though it is more expensive and less readily available.
Blood Tests
A complete blood count may reveal anemia, which may be caused either by blood loss or vitamin B12 deficiency. The latter may be seen with ileitis because vitamin B12 is absorbed in the ileum. Erythrocyte sedimentation rate, or ESR, and C-reactive protein measurements can also be useful to gauge the degree of inflammation.[48] It is also true in patient with ilectomy done in response to the complication. Another cause of anaemia is anaemia of chronic disease, characterized by its microcytic and hypochromic anaemia. There are reasons in anaemia, including medication in treatment of inflammatory bowel disease like azathioprine can lead to cytopenia and sulfasalazine can also result in folate malabsorption, etc. Testing for anti-Saccharomyces cerevisiae antibodies (ASCA) and anti-neutrophil cytoplasmic antibodies (ANCA) has been evaluated to identify inflammatory diseases of the intestine and to differentiate Crohn’s disease from ulcerative colitis.
Treatment:
Crohn’s is a chronic inflammatory disease of the bowel and treatment is focused on reducing inflammation. Treatment options include medications, nutritional supplements and surgery—either alone or in combination. Complementary and alternative treatments are used to help relieve symptoms in conjunction with other therapies. Treating Crohn’s disease effectively is complex – goals of therapy are to alleviate symptoms and to prevent flare-ups. It is important to develop a strong partnership with your gastroenterologist and nutritionist.
Medications: Aminosalicylates (sulfasalazine, mesalamine, balsalazide, and olsalazine) are given orally or rectally to reduce inflammation in the intestine. Corticosteroids (prednisone, methylprednisolone, hydrocortisone) reduce inflammation and are used short-term for acute flareups. Budesonide, one of a new class of nonsystemic steroids, targets the intestine rather than the whole body. Immunomodulators (azathioprine, 6-mercaptopurine, cyclosporine A, tacrolimus, methotrexate ), usually associated with organ transplants and used to decrease the risk of rejection. Increasingly, they’re being used to treat autoimmune diseases and used to treat people with Crohn’s disease. Usually prescribed for moderate to severe cases, immunomodulators are also used when fistulas develop or corticosteroids are no longer effective. Crohn’s is not caused by an infection, but antibiotics (metronidazole and ciprofloxacin) may help minimize symptoms and heal fistulas and abscesses. Biologics (infliximab (Remicade), adalimumab (Humira) are genetically engineered drugs that combat inflammation by neutralizing proteins in the immune system like tumor necrosis factor (TNF), which can cause inflammation. The advantage in using biologics is that they act selectively rather than suppressing the entire immune system.
Nutritional Support: Nutritional support for people with Crohn’s is a complex endeavor. Malnutrition is a common complication of the illness. Children need to increase their intake of calories and protein by as much as 150% of the recommended amounts for their age and height. It’s also important to increase fluids, proteins (especially fatty fish like tuna and salmon), complex carbohydrates, and potassium-rich foods like bananas, orange juice, potatoes and avocados. Supplements like fish oils, probiotics and liquid nutritional support (Ensure) may help, so be sure to consult your health professionals for the best plan for you or your child.
Complementary and Alternative Therapies:Many people are interested in nontraditional approaches to healing, especially when standard treatments produce intolerable side effects or aren’t able to provide an improvement. To address this interest, the National Institutes of Health established the National Center for Complementary and Alternative Medicine (NCCAM), which provides guidance and research.
Most complementary and alternative therapies don’t simply address a problem with the body. Instead, they focus on the entire person – body, mind and spirit. As a result, they can be especially effective at reducing stress, alleviating the side effects of conventional treatments and improving quality of life.
Studies have found that more than half the people with either Crohn’s disease or ulcerative colitis have used some form of complementary or alternative therapy. The most common complementary therapies tried were herbal and nutritional supplements, probiotics and fish oil. Side effects and ineffectiveness of conventional therapies are primary reasons for seeking alternative care. Only about two-thirds report their alternative or complementary therapy use to their doctors, however.
The majority of these therapies aren’t regulated as medications by the Food and Drug Administration. Manufacturers can claim that their therapies are safe and effective but don’t need to prove it. Because even natural herbs can have side effects and cause dangerous interactions, be sure to let your doctor know before you try any alternative or complementary therapies.
NCCAM’s findings are available on its Web site. You can also talk to information specialists at the center’s clearinghouse by calling 888-644-6226 between 8:30 a.m. and 5 p.m. Eastern time.
Moderate, regular exercise and stress management techniques like meditation, relaxation practices and cognitive therapy may help reduce the severity of symptoms.
Click to see also:>Alternative strategy better for Crohn’s Disease
Ayurvedic Recommended Therapy: Basti
Homeopathy – Crohn’s Disease And It’s Treatment…………..(1)…….(2)
Crohn’s Disease as related to Cat’s Claw
Lifestyle changes:
Certain lifestyle changes can reduce symptoms, including dietary adjustments, proper hydration and smoking cessation.
Surgery: Most people with Crohn’s disease eventually need some type of surgery. Half of all children diagnosed with Crohn’s need surgery within 5 years. Surgery is used to remove damaged portions of the digestive tract or scar tissue or repair fistulas. Strictureplasty involves insertion of a ballon to widen narrow segments of intestine without having to remove any portion. Resection of the colon is done to remove damaged intestine. Subtotal colectomy removes part of the colon. Proctocolectomy removes the entire colon. An ileostomy is the creation of a stoma through which feces is passed and collected in a bag which must be emptied several times per day. Emergency surgery is sometimes required for bowel perforations, obstructions, intestinal bleeding, or severe fistulas.
Prospective Treatments:
Researchers at University College London have questioned the wisdom of suppressing the immune system in Crohn’s, as the problem may be an under-active rather than an over-active immune system: their study found that Crohn’s patients showed an abnormally low response to an introduced infection, marked by a poor flow of blood to the wound, and the response improved when the patients were given sildenafil.
Recent studies using helminthic therapy or hookworms to treat Crohn’s Disease and other (non-viral) auto-immune diseases seem to yield promising results.
A single, small, uncontrolled trial of patients with mild Crohn’s on stable medications suggested improvement with low dose naltrexone therapy.
Prognosis:
Crohn’s disease is a chronic condition for which there is currently no cure. It is characterized by periods of improvement followed by episodes when symptoms flare up. With treatment, most people achieve a healthy height and weight, and the mortality rate for the disease is low.
Crohn’s disease is a recurring disorder. Most affected people learn to live reasonably normal lives, but 7 in 10 people eventually need surgery. Complications and repeated surgery can occasionally reduce life expectancy. Crohn’s disease may increase the risk of colorectal cancer, and, for this reason, your doctor may advise you to have regular checkups that include colonoscopy.
Disclaimer: This information is not meant to be a substitute for professional medical advise or help. It is always best to consult with a Physician about serious health concerns. This information is in no way intended to diagnose or prescribe remedies.This is purely for educational purpose.
Resources:
http://www.healthline.com/humiracontent/crohn’s-disease-advanced-treatments
http://www.charak.com/DiseasePage.asp?thx=1&id=108
http://en.wikipedia.org/wiki/Crohn’s_disease
http://www.mayoclinic.com/health/crohns-disease/DS00104/DSECTION=11
One reply on “Crohn’s Disease”
[…] new study has discovered that nutritional supplements with vitamin D could help fight Crohn’s disease, which is a chronic form of inflammatory bowel […]