Alternative Names :Toxic diffuse goiter, thyrotoxicosis,diffuse thyrotoxic goiter
Definition:
Graves’ disease is the most common cause of hyperthyroidism . Hyperthyroidism is an autoimmune disorder that occurs when the thyroid gland makes more thyroid hormone than the body needs.
The thyroid is a small, butterfly-shaped gland in the front of the neck below the larynx, or voice box. The thyroid gland makes two thyroid hormones, triiodothyronine (T3) and thyroxine (T4). Thyroid hormones affect metabolism, brain development, breathing, heart and nervous system functions, body temperature, muscle strength, skin dryness, menstrual cycles, weight, and cholesterol levels.
Thyroid hormone production is regulated by another hormone called thyroid-stimulating hormone (TSH), which is made by the pituitary gland located in the brain.
Graves’ disease is an autoimmune disorder, meaning the body’s immune system acts against its own healthy cells and tissues. In Graves’ disease, the immune system makes antibodies called thyroid-stimulating immunoglobulin (TSI) that attach to thyroid cells. TSI mimics the action of TSH and stimulates the thyroid to make too much thyroid hormone. Sometimes the antibodies can instead block thyroid hormone production, leading to a confusing clinical picture. The diagnosis and treatment of Graves’ disease is often performed by an endocrinologist—a doctor who specializes in the body’s hormone-secreting glands.
Graves’ disease is rarely life-threatening. Although it may develop at any age and in either men or women, Graves’ disease is more common in women and usually begins after age 20.
Recent studies in England put the incidence of Graves’ disease at 1 to 2 cases per 1,000 population per year (in England). It occurs much more frequently in women than in men. The disease frequently presents itself during early adolescence or begins gradually in adult women, often after childbirth, and is progressive until treatment. It has a powerful hereditary component.
Graves’ disease tends to be more severe in men, even though it is rarer. It appears less likely to go into permanent remission and the eye disease tends to be more severe, but men are less likely to have large goitres. In a statistical study of symptoms and signs of 184 thyrotoxic patients (52 men, 132 women), the male patients were somewhat older than the females, and there were more severe cases among men than among women. Cardiac symptoms were more common in women, even though the men were older and more often had a severe form of the disease; palpitations and dyspnea were more common and severe in women.
Cigarette smoking, which is associated with many autoimmune diseases, raises the incidence of Graves’ ophthalmopathy 7.7-fold.
There’s no way to stop your immune system from attacking your thyroid gland, but treatments for Graves’ disease can ease symptoms and decrease the production of thyroxine.
Symptoms:
Graves’ disease symptoms may include:
*Anxiety
*Difficulty sleeping
*Fatigue
*A rapid or irregular heartbeat
*A fine tremor of your hands or fingers
*An increase in perspiration
*Sensitivity to heat
*Weight loss, despite normal food intake
*Brittle hair
*Enlargement of your thyroid gland (goiter)
*Change in menstrual cycles
*Frequent bowel movements
*Increased appetite
*Diarrhoea
*Tremor and shaking
*Irritability and emotional upsets
*Profuse sweating
*Dislike of hot weather
*Itching, reddening and thickening of the skin, typically over the shins
Graves’ ophthalmopathy
It’s also fairly common for your eyes to exhibit mild signs of a condition known as Graves’ ophthalmopathy. In Graves’ ophthalmopathy, your eyeballs bulge out past their protective orbit (exophthalmos). This occurs as tissues and muscles behind your eyes swell and cause your eyeballs to move forward. Because your eyes may be pushed so far forward, the front surface of your eyes can become dry. Cigarette smokers with Graves’ disease are five times more likely than nonsmokers to develop Graves’ ophthalmopathy. This is possibly because smoking inhibits the absorption of anti-thyroid medication that is used to treat Graves’ disease.
Graves’ ophthalmopathy may cause these mild signs and symptoms:
*Excess tearing and sensation of grit or sand in either or both eyes
*Reddened or inflamed eyes
*Widening of the space between your eyelids
*Swelling of the lids and tissues around the eyes
*Light sensitivity
.
Less often, Graves’ ophthalmopathy can produce these serious signs and symptoms:
*Ulcers on the cornea
*Double vision
*Limited eye movements
*Blurred or reduced vision
There may also be a goitre (or swelling of the thyroid gland in the neck) and swelling of the tissues over the front of the shins.
Cause:
The trigger for autoantibody production is unknown.
Since Graves’ disease is an autoimmune disease which appears suddenly, often quite late in life, it is thought that a viral or bacterial infection may trigger antibodies which cross-react with the human TSH receptor (a phenomenon known as antigenic mimicry, also seen in some cases of type I diabetes)[citation needed]. One possible culprit is the bacterium Yersinia enterocolitica (not the same as Yersinia pestis, the agent of bubonic plague). However, although there is indirect evidence for the structural similarity between the bacterium and the human thyrotropin receptor, direct causative evidence is limited. Yersinia seems not to be a major cause of this disease, although it may contribute to the development of thyroid autoimmunity arising for other reasons in genetically susceptible individuals. It has also been suggested that Y. enterocolitica infection is not the cause of auto-immune thyroid disease, but rather is only an associated condition; with both having a shared inherited susceptibility. More recently the role for Y. enterocolitica has been disputed.
Some of the eye symptoms of hyperthyroidism are believed to result from heightened sensitivity of receptors to sympathetic nervous system activity, possibly mediated by increased alpha-adrenergic receptors in some tissues.
Like most auto-immune conditions, women seem to be far more susceptible. Graves is up to eight times more common in women than men.
Some people may have a genetic predisposition to develop TSH receptor autoantibodies. HLADR (especially DR3) appears to play a significant role.
Risk Factors:
It’s known there are links between autoimmune conditions, so Graves’ disease is linked to insulin-dependent diabetes and pernicious anaemia (which are classed as autoimmune conditions). So when a person has one of these, they or members of their family may be at increased risk of developing another.
There’s also a genetic influence contributing to Graves’ disease and it can run in families.
Diagnosis:-
The onset of Graves’ disease symptoms is often insidious: the intensity of symptoms can increase gradually for a long time before the patient is correctly diagnosed with Graves’ disease, which may take months or years. (Not only Graves’ disease, but most endocrinological diseases have an insidious, subclinical onset.) One study puts the average time for diagnosis at 2.9 years, having observed a range from 3 months to 20 years in their sample population. A 1996 study offers a partial explanation for this generally late diagnosis, suggesting that the psychiatric symptoms (due to the hyperthyroidism) appeared to result in delays in seeking treatment as well as delays in receiving appropriate diagnosis. Also, earlier symptoms of nervousness, hyperactivity, and a decline in school performance, may easily be attributed to other causes.[citation needed] Many symptoms may occasionally be noted, at times, in otherwise healthy individuals who do not have thyroid disease (e.g., everyone feels anxiety and tension to some degree), and many thyroid symptoms are similar to those of other diseases. Thus, clinical findings may be full blown and unmistakable or insidious and easily confused with other disorders. The results of overlooking the thyroid can however be very serious. Also noteworthy and problematic, is that in a 1996 survey study respondents reported a significant decline in memory, attention, planning, and overall productivity from the period 2 years prior to Graves’ symptoms onset to the period when hyperthyroid.[28] Also, hypersensitivity of the central nervous system to low-grade hyperthyroidism can result in an anxiety disorder before other Graves’ disease symptoms emerge. E.g., panic disorder has been reported to precede Graves’ hyperthyroidism by 4 to 5 years in some cases, although it is not known how frequently this occurs.
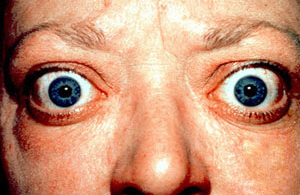
The resulting hyperthyroidism in Graves’ disease causes a wide variety of symptoms. The two signs that are truly ‘diagnostic’ of Graves’ disease (i.e., not seen in other hyperthyroid conditions) are exophthalmos (protuberance of one or both eyes) and pretibial myxedema, a rare skin disorder with an occurrence rate of 1-4%, that causes lumpy, reddish skin on the lower legs. Graves’ disease also causes goitre (an enlargement of the thyroid gland) that is of the diffuse type (i.e., spread throughout the gland). This phenomenon also occurs with other causes of hyperthyroidism, though Graves’ disease is the most common cause of diffuse goitre. A large goitre will be visible to the naked eye, but a smaller goitre (very mild enlargement of the gland) may be detectable only by physical exam. Occasionally, goitre is not clinically detectable but may be seen only with CT or ultrasound examination of the thyroid.
A highly suggestive symptom of hyperthyroidism, is a change in reaction to external temperature. A hyperthyroid person will usually develop a preference for cold weather, a desire for less clothing and less bed covering, and a decreased ability to tolerate hot weather. When thyroid disease runs in the family, the physician should be particularly wary: studies of twins suggest that the genetic factors account for 79% of the liability to the development of Graves’ disease (whereas environmental factors account presumably for the remainder). Other nearly pathognomonic signs of hyperthyroidism are excessive sweating, high pulse during sleep, and a pattern of weight loss with increased appetite (although this may also occur in diabetes mellitus and malabsorption or intestinal parasitism).
Hyperthyroidism in Graves’ disease is confirmed, as with any other cause of hyperthyroidism, by a blood test. Elevated blood levels of the principal thyroid hormones (i.e. free T3 and T4), and a suppressed thyroid-stimulating hormone (low due to negative feedback from the elevated T3 and T4), point to hyperthyroidism
However, a 2007 study makes clear that diagnosis depends to a considerable extent on the position of the patient’s unique set point for T4 and T3 within the laboratory reference range (an important issue which is further elaborated below).
Differentiating Graves’ hyperthyroidism from the other causes of hyperthyroidism (thyroiditis, toxic multinodular goiter, toxic thyroid nodule, and excess thyroid hormone supplementation) is important to determine proper treatment. Thus, when hyperthyroidism is confirmed, or when blood results are inconclusive, thyroid antibodies should be measured. Measurement of thyroid stimulating immunoglobulin (TSI) is the most accurate measure of thyroid antibodies. They will be positive in 60 to 90% of children with Graves’ disease. If TSI is not elevated, then a radioactive iodine uptake should be performed; an elevated result with a diffuse pattern is typical of Graves’ disease. Biopsy to obtain histological testing is not normally required but may be obtained if thyroidectomy is performed.
Treatment :
Treatment aims to:
•Keep thyroid hormone levels in the normal range
•Prevent eye problems (which can result from exposure of the delicate eye tissues in Graves’ opthalmopathy) – this can be very difficult and eye symptoms may persist even when treatments work well to keep thyroid hormone levels within the normal range.
.
Treatment for the raised hormone levels can include:
•Drugs for immediate and then long-term control
•Surgery to remove part of the thyroid gland
•Radioactive iodine treatment (RAI)
.
In recent years, efforts have been made to find a dose of RAI that will give a good cure rate for thyrotoxicosis without leading to underactivity (known as hypothyroidism). However, this has proved difficult and hypothyroidism remains a side-effect of the treatment, affecting as many as 20 per cent of those treated within the first couple of years after treatment, and three to five per cent more each year after that.
Those affected may need lifelong supplements of thyroid hormones.
Treatment for the eye problems includes:
•Drug treatments and eye drops to reduce swelling and close lids
•Steroids, especially if the eye muscles are paralysed or the swelling is very bad
•Surgery to reduce swelling or closed lids
•Radiotherapy is sometimes used in difficult cases.
.
Neuropsychiatric symptoms:
A substantial proportion of patients have an altered mental state, even after successful treatment of hyperthyroidism. When psychiatric disorders remain after restoration of euthyroidism and after treatment with beta blockers, specific treatment for the psychiatric symptoms, especially psychotropic drugs, may be needed.[10] A literature study concluded in 2006, found that, after being diagnosed with Graves’ hyperthyroidism, approximately one-third of patients are prescribed psychotropic drugs. Sometimes these drugs are given to treat mental symptoms of hyperthyroidism, sometimes to treat mental symptoms remaining after amelioration of hyperthyroidism, and sometimes when the diagnosis of Graves’ hyperthyroidism has been missed and the patient is treated as having a primary psychiatric disorder. There are no systematic data on the general efficacy of psychotropic drugs in the treatment of mental symptoms in patients with hyperthyroidism, although many reports describe the use of individual agents. De Groot mentions that a mild sedative or tranquilizer is often helpful. German research of 2004 reported that 35 percent of treated Graves’ disease patients (with normal thyroid tests for at least six months after treatment), suffered from psychological distress, and had high levels of anxiety. Almost all these patients had clear-cut depression
General measurements:
Graves’ disease patients are nutritionally depleted in proportion to the duration and severity of their illness. Until metabolism is restored to normal, and for some time afterward, caloric and protein requirements may be well above normal. Specific deficiencies may exist, and multivitamin supplementation is indicated. The intake of calcium should be above normal. All in all, the physician should pay heed to the patient’s emotional needs, as well as to his or her requirements for rest, nutrition, and specific (anti)thyroid medication
Prognosis:
The disease typically begins gradually, and is progressive unless treated. If left untreated, more serious complications could result, including bone loss and fractures, inanition, birth defects in pregnancy, increased risk of a miscarriage. Graves disease is often accompanied by an increase in heart rate, which may lead to cardiovascular damage and further heart complications including loss of the normal heart rhythm (atrial fibrillation), which may lead to stroke. If the eyes are bulging severely enough that the lids do not close completely at night, severe dryness will occur with a very high risk of a secondary corneal infection which could lead to blindness. Pressure on the optic nerve behind the globe can lead to visual field defects and vision loss as well. In severe thyrotoxicosis, a condition frequently referred to as thyroid storm, the neurologic presentations are more fulminant, progressing if untreated through an agitated delirium to somnolence and ultimately to coma. All in all, untreated Graves’ disease can lead to significant morbidity, disability and even death. However, the long-term history also includes spontaneous remission in some cases and eventual spontaneous development of hypothyroidism if autoimmune thyroiditis coexists and destroys the thyroid gland.
When effective thyroid treatment is begun, the general response is quite favorable: physical symptoms resolve, vitality returns and the mental processes become efficient again. However, symptom relief is usually not immediate and is achieved over time as the treatments take effect and thyroid levels reach stability. In addition, not all symptoms may resolve at the same time. Prognosis also depends on the duration and severity of the disease before treatment. Swedish research of 2005 reports a lower quality of life for 14 to 21 years after treatment of Graves’ disease, with lower mood and lower vitality, regardless of the choice of treatment.
Remission and relapses:
A literature study in 2006 found that patients who have residual mental symptoms have a significantly higher chance of relapse of hyperthyroidism. Patients with recurrent Graves’ hyperthyroidism, compared with patients in remission and healthy subjects, had significantly higher scores on scales related to depression and anxiety, as well as less tolerance of stress. According to a 2010 publication, a total thyroidectomy offers the best chance of preventing recurrent hyperthyroidism.
Mental impairment:
A literature review in 2006, whilst noting methodology issues in the consistency of Graves’ disease diagnostic criteria, found many reports about residual complaints in patients who were euthyroid after treatment with a high prevalence of anxiety disorders and bipolar disorder, as well as elevated scores on scales of anxiety, depression and psychological distress. Bunevicius et al. point out that this “substantial mental disability” is more severe in patients with residual hyperthyroidism but is present even in euthyroid patients. Delay in therapy markedly worsens the prognosis for recovery, but complications can be prevented by early treatment. In rare cases, patients will experience psychosis-like symptoms only after they have been treated for hypo- or hyperthyroidism, due to a rapid normalisation of thyroid hormone levels in a patient who has partly adapted to abnormal values.
Thyroid replacement treatment after thyroidectomy or radioiodine:
Several studies find a high frequency of TSH level abnormalities in patients who take thyroid hormone supplemenation for long periods of time, and stress the importance of periodic assessment of serum TSH.
Possible Complications:-
*Complications from surgery, including:
*Hoarseness from damage to the nerve leading to the voice box
*Low calcium levels from damage to the parathyroid glands (located near the thyroid gland)
*Scarring of the neck
*Eye problems (called Graves ophthalmopathy or exophthalmos)
•Heart-related complications, including:
*Rapid heart rate
*Congestive heart failure (especially in the elderly)
*Atrial fibrillation
*Thyroid crisis (thyrotoxic storm), a severe worsening of overactive thyroid gland symptoms
*Increased risk for osteoporosis, if hyperthyroidism is present for a long time
•Complications related to thyroid hormone replacement
*If too little hormone is given, fatigue, weight gain, high cholesterol, depression, physical sluggishness, and other symptoms of hypothyroidism can occur
*If too much hormone is given, symptoms of hyperthyroidism will return
Lifestyle and Home Remedies:
For Graves’ ophthalmopathy
These steps may make your eyes feel better if you have Graves’ ophthalmopathy:
*Apply cool compresses to your eyes. The added moisture may soothe your eyes.
*Wear sunglasses. When your eyes protrude, they’re more vulnerable to ultraviolet rays and more sensitive to bright light. Wearing sunglasses that wrap around the sides of your head will lessen the irritation of your eyes from the wind.
*Use lubricating eyedrops. Eyedrops may relieve the dry, scratchy sensation on the surface of your eyes. At night, a paraffin-based gel such as Lacri-Lube can be applied.
*Elevate the head of your bed. Keeping your head higher than the rest of your body lessens fluid accumulation in the head and may relieve the pressure on your eyes.
For Graves’ dermopathy
If the disease affects your skin (Graves’ dermopathy), use over-the-counter creams or ointments containing hydrocortisone to relieve swelling and reddening. In addition, using compression wraps on your legs may help.
Coping and support:
If you have Graves’ disease, make your mental and physical well-being a priority. Eating well and exercising can enhance the improvement in some symptoms while being treated and help you feel better in general. For example, because your thyroid controls your metabolism, you may have a tendency to gain weight when the hyperthyroidism corrects. Brittle bones can also occur with Graves’ disease and weight-bearing exercises can help maintain bone density.
Try to ease stress as much as you can, as stress possibly contributes to the development of Graves’ disease. Listening to music, taking a warm bath or walking can help relax you and put you in a better frame of mind. Partner with your doctor to construct a plan that incorporates good nutrition, exercise and relaxation into your daily routine.
Disclaimer: This information is not meant to be a substitute for professional medical advise or help. It is always best to consult with a Physician about serious health concerns. This information is in no way intended to diagnose or prescribe remedies.This is purely for educational purpose.
Resources:
http://www.bbc.co.uk/health/physical_health/conditions/gravesdisease.shtml
http://www.nlm.nih.gov/medlineplus/ency/article/000358.htm
http://en.wikipedia.org/wiki/Graves’_disease
http://www.mayoclinic.com/health/graves-disease/DS00181
http://www.nlm.nih.gov/medlineplus/ency/imagepages/17067.htm
http://endocrine.niddk.nih.gov/pubs/graves/#symptoms
Related articles
- Can I take 5mg methimazole for Graves Disease for life (zocdoc.com)
- Does someone with Graves rash have Graves’ Disease? (zocdoc.com)
- Are goiters a type of thyroid cancer? (zocdoc.com)
- Can Hashimoto’s disease occur at any age? (zocdoc.com)
- At what TSH level would you recommend medication for the treatment of hyperthyroidism? (zocdoc.com)
- Causes of Hyperthyroidism (brighthub.com)





