The knee has a simple purpose. It needs to flex (bend) or extend (straighten) to allow the body to perform many activities like running, walking, kicking, and sitting. Imagine standing up from a chair if your knees couldn’t bend.
Knee Anatomy…
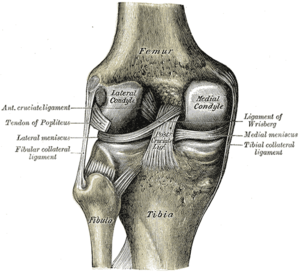
While there are four bones that come together at the knee, only the femur (thigh bone) and the tibia (shin bone) form the joint itself. The head of the fibula (strut bone on the outside of the leg) provides some stability, and the patella (kneecap) helps with joint function. Movement and weight-bearing occur where the ends of the femur called the femoral condyles match up with the top flat surfaces of the tibia (tibial plateaus).
There are two major muscle groups that are balanced and allow movement of the knee joint. Contracting the quadriceps muscles on the front of the thigh extends the knee, while the hamstring muscles on the back of the thigh flex the knee when they contract. The muscles cross the knee joint and are attached to the tibia by tendons. The quadriceps tendon is a little special, in that it contains the patella within it. The patella allows the quadriceps muscle/tendon unit to work more efficiently. This tendon is renamed the patellar tendon in the area below the kneecap to its attachment to the tibia.
The stability of the knee joint is maintained by four ligaments, thick bands of tissue that stabilize the joint. The medial collateral ligament (MCL) and lateral collateral ligament (LCL) are on the sides of the knee and prevent the joint from sliding sideways. The anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) form an “X” on the inside of the knee and prevent the knee from sliding back and forth. These limitations on knee movement allow the knee to concentrate the forces of the muscles on flexion and extension.
Inside the knee, there are two shock-absorbing pieces of cartilage called menisci (singular meniscus) that sit on the top surface of the tibia. The menisci allow the femoral condyle to move on the tibial surface without friction, preventing the bones from rubbing on each other.
Bursas surround the knee joint and are fluid filled sacs that cushion the knee during its range of motion. In the front of the knee, there is a bursa between the skin and the kneecap called the prepatellar bursa and another above the kneecap called the suprapatellar bursa (supra=above).
Each part of the anatomy needs to function properly for the knee to work. Acute injury and trauma as well as chronic overuse can both cause inflammation and its accompanying symptoms of pain, swelling, redness and warmth.
Causes: ..
.. ..
.. .
.
While direct blows will occur, the knee is more susceptible to twisting or stretching injuries, taking the joint through a greater range of motion than it can tolerate.
If the knee is stressed from a specific direction, then the ligament trying to hold it in place against that force can tear. Ligament stretching or tears are called sprains. These sprains are graded as first, second, or third degree based upon how much damage has occurred. Grade one sprains stretch the ligament but don’t tear the fibers; grade two sprains partially tear the fibers, but the ligament remains intact; and grade three tears completely disrupt the ligament.
Twisting injuries to the knee put stress on the cartilage or meniscus and can pinch it between the tibial surface and the edges of the femoral condyle, causing tears.
Injuries of the muscles and tendons surrounding the knee are caused by acute hyperflexion or hyperextension of the knee or by overuse. These injuries are called strains.
There can be inflammation of the bursas (known as bursitis) of the knee that can occur because of direct blows or chronic use and abuse.
Acute knee injuries fall into two groups; those where there is almost immediate swelling in the joint associated with the inability to bend the knee and bear weight, and those where there is discomfort and perhaps localized pain to one side of the knee, but have minimal swelling and minimal effects on walking.
Symptoms:
Acute knee injuries can cause pain and swelling with difficulty bending the knee and weight-bearing.
Longer-term symptoms that point to knee problems will include pain and swelling in addition to other complaints. Inflammation in the joint may be caused by even minor activity. Swelling may be intermittent, brought on by activity, and may gradually resolve as the inflammation decreases.
Pain, too, may come and go and may not occur right away with activity but might be delayed as the inflammation develops. Pain can also be felt with specific activities. Pain while climbing stairs is a symptom of meniscus injury, where the cartilage is being pinched in the joint as it narrows with bending. Pain with walking down stairs suggests patellar pain, where the kneecap is being forced onto the femur.
Giving way, or a feeling of instability, of the knee is a symptom of ligament injury, while popping or grinding in the knee is more associated with cartilage or meniscus tears. “Locking” is the term used when the knee joint refuses to completely straighten, and this is always due to torn cartilage. In this situation, the torn piece of cartilage folds upon itself and doesn’t allow the knee to extend.
Emergent medical care should be sought if, due to injury,
1.there is almost immediate swelling in the knee,
2.if the bones appear deformed,
3.if there is inability to bear weight,
4.if the pain is intolerable,
5.if there is loss of sensation below the injury site
6.or if the foot and ankle turn cold and no pulses can be felt.
Diagnosis:
The initial evaluation by the physician or health care provider will begin with a medical history. Whether the evaluation is occurring immediately after the injury or weeks later, the physician will ask about the mechanism of injury to help isolate what structures in the knee might be damaged. Is the injury due to a direct blow that might suggest a fracture or contusion or bruise? Was it a twisting injury that causes a cartilage or meniscus tear? Was there an injury associated with a planted foot to place stress and potentially tear a ligament?
Further questions will address other symptoms. Was swelling present, and if so, did it occur right away or was it delayed by hours? Did the injury prevent weight-bearing or walking? Does going up or down steps cause pain? Is there associated hip or ankle pain?
Physical examination of the knee begins with inspection, in which the physician will look at the bones and make certain they are where they belong. With fractures of the kneecap or patellar tendon injuries, the kneecap can slide high out of position. Also, patellar dislocations, where the kneecap slides to the outside or lateral part of the knee, are easily evident on inspection. Looking at how the knee is held is also important. If the knee is held slightly flexed, it can be a clue that there is fluid in the joint space, since joint space is maximal at 15 degrees of flexion.
Palpation (feeling) is the next part of the exam, and knowing the anatomy, the physician can feel where any pain might exist and correlate that to the underlying structures like ligaments or muscle-insertion points. Palpation over the joint line, the space between the bones in the front part of the knee, can show fluid or tenderness associated with meniscus injury. This is also the part of the exam where the ligaments are stressed to make certain that they are intact. Sometimes, the physician will also stress the uninjured knee to see how loose or tight the normal ligaments are as a comparison. Finally, the blood supply and nerve supply to the leg and foot will be assessed.
Sometimes x-rays of the knee are required to make certain there are no broken bones, but often with stress or overuse injuries where no direct blow has occurred, plain x-rays are not needed and imaging of the knee may wait until a later date, where an MRI might be considered.
Treatment:
Almost all knee injuries will need more than one visit to the doctor. If no operation is indicated, then RICE (rest, ice, compression, and elevation) with some strengthening exercises and perhaps physical therapy will be needed. Sometimes the decision for surgery is delayed to see if the RICE and physical therapy will be effective. Each injury is unique, and treatment decisions depend on what the expectation for function will be. As an example, a torn ACL would usually require surgery in a young athlete, but the ACL may be allowed to heal with physical therapy in an 80-year-old who is not very mobile.
With the technology available, many knee injuries that require surgery can be treated surgically with an arthroscope, where a camera is used and small punctures are made in the knee to insert instruments. Patients usually begin their post-op rehabilitation within days of the surgery.
Sometimes surgery is delayed to allow the patient to strengthen the muscles around the knee joint. If there is no rush to operate, then opportunity exists to strengthen the quadriceps and hamstring muscles beforehand to allow for easier post-operative therapy.
Diagnosis and Treatment of Specific Types of Knee Injuries
Muscle Tendon Injuries:-Almost all of these strains are treated with ice, elevation and rest. Sometimes compression with an ace wrap or knee sleeve is recommended, and crutches may be used for a short time to assist with walking. Ibuprofen can be used as an anti-inflammatory medication.
The mechanism of injury is either hyperextension, in which the hamstring muscles can be stretched or torn, or hyperflexion, in which the quadriceps muscle is injured. Rarely with a hyperflexion injury, the patellar or quadriceps tendon can be damaged and rupture. This injury is characterized by the inability to extend the knee and a defect that can be felt either above or below the patella. Surgery is required to repair this injury.
MCL and LCL Injuries
These ligaments can be stretched or torn when the foot is planted and a sideways force is directed to the knee. This can cause significant pain and difficulty walking as the body tries to protect the knee, but there is usually little swelling within the knee. The treatment for this injury may include a knee immobilizer, a removable Velcro splint that keeps the knee straight and keeps the knee stable. RICE (rest, ice, compression, and elevation) are the mainstays of treatment.
ACL Injuries
If the foot is planted and there is force applied from the front to back to the knee, then the cruciate ligaments can be damaged. Swelling in the knee occurs within minutes, and attempts at walking are difficult. The definitive diagnosis is difficult in the emergency department because the swelling and pain make it hard to test if the ligament is loose. Long-term treatment may require surgery and significant physical therapy to return good function of the knee joint.
Mensicus Tears
The cartilage of the knee can be acutely injured or can gradually tear. Acutely, the injury is of a twisting nature where the cartilage that is attached to and lays flat on the tibia is pinched between the femoral condyle and the tibial plateau. Pain and swelling occur gradually over many hours (as opposed to an ACL tear which swells much more quickly). Sometimes the injury seems trivial and no care is sought, but chronic pain occurs over time. There may be intermittent swelling, pain with walking uphill or climbing steps or giving way of the knee that results in near falls. History and physical examination often can make the diagnosis and MRI may be used to confirm it.
Fractures
Fractures of the bones of knee are relatively common. The patella, or kneecap, may fracture due to a fall directly onto it or in car accidents, when the knee is driven into the dashboard. If the bone is pulled apart, surgery will be required for repair, but if the bone is in good position, a knee immobilizer and watchful waiting may be all that is required.
The head of the fibula on the lateral side of the knee joint can be fractured either by a direct blow or as part of an injury to the shin or ankle. This bone usually heals with little intervention, but fractures of this bone can have a major complication. The peroneal nerve wraps around the bone and can be damaged by the fracture. This will cause a foot drop, so do not be surprised if the physician examines your foot when you complain of knee problems.
With jumping injuries, the surface of the tibia can be damaged, resulting in a fracture to the tibial plateau. Since this is where the femoral condyle sits to move the knee joint, it is important that it heals in the best position possible. For that reason, after plain x-rays reveal this fracture, a CT scan is done to make certain that there is no displacement of the bones. Occasionally this type of fracture requires surgery for repair.
Fractures of the femur require significant force, but in people with osteoporosis, less force is needed to cause a fracture of this large bone. In people with knee replacements who fall, there is a potential weakness at the site of the knee replacement above the femoral condyle, and this can be a site of fracture. The decision to operate or treat by immobilization with a cast will be made by the orthopedist.
Bursa Inflammation
Housemaid’s knee (prepatellar bursitis) is due to repetitive kneeling and crawling on the knees. The bursa or space between the skin and kneecap becomes inflamed and fills with fluid. It is a localized injury and does not involve the knee itself. Treatment includes padding the knee and using ibuprofen as an anti-inflammatory medication.
Patellar Injuries
The kneecap sits within the tendon of the quadriceps muscle, in front of the femur, just above the knee joint. It is held in place by the muscles of the knee.
The patella can dislocate laterally (toward the outside of the knee). This occurs more commonly in women because of anatomic differences in the angle aligning the femur and tibia. Fortunately, the dislocation is easily returned to the normal position by straightening out the knee, usually resulting in the kneecap popping into place. Unfortunately, physical therapy and muscle strengthening are needed to prevent recurrent dislocations.
Patello-femoral syndrome occurs when the underside of the patella becomes inflamed if irritation develops as it rides its path with each flexion and extension of the knee, and it does not track smoothly. This inflammation can cause localized pain, especially with walking down stairs and with running. Treatment includes ice, anti-inflammatory medication, and exercises to balance the quadriceps muscle. More severe cases may require arthroscopic surgery to remove some of the inflamed cartilage and realign parts of the quadriceps muscle.
Click to see to learn more:->………..(1)….(2)…..(3)……(4)....(5)…..(6)…(7)
Prevention:
Accidents happen, and while many knee injuries occur during recreational activities or sports, more happen at work and at home.
Strong muscles stabilize joints. With the knee, having strong and flexible quadriceps and hamstring muscles can prevent minor stresses to the knee from causing significant injury.
Proper footwear can also minimize the risk for knee injury. Wearing shoes that are appropriate for the activity can lessen the risk of twisting and other forces that can stress the knee.
Disclaimer: This information is not meant to be a substitute for professional medical advise or help. It is always best to consult with a Physician about serious health concerns. This information is in no way intended to diagnose or prescribe remedies.This is purely for educational purpose


![Reblog this post [with Zemanta]](https://i0.wp.com/img.zemanta.com/reblog_e.png?w=580)








 ..
.. ..
.. .
.