Alternative Names: Seborrheic eczema; Cradle cap,infantile or neonatal seborrhoeic dermatitis,
crusta lactea, milk crust, honeycomb disease.
Definition:
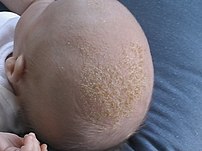
Cradle cap is a yellowish, patchy, greasy, scaly and crusty skin rash that occurs on the scalp of recently born babies. It is usually not itchy, and does not bother the baby. Cradle cap most commonly begins sometime in the first 3 months. Similar symptoms in older children are more likely to be dandruff than cradle cap. The rash is often prominent around the ear, the eyebrows or the eyelids. It may appear in other locations as well, where it is called seborrhoeic dermatitis rather than cradle cap. Some countries use the term pityriasis capitis for cradle cap. It is extremely common, with about half of all babies affected. Most of them have a mild version of the disorder. Severe cradle cap is rare.
CLICK & SEE
It’s not due to poor hygiene and isn’t contagious or an allergy. Cradle cap tends to run in families, so there may be a genetic predisposition.
Cradle cap usually resolves on its own within a few months. Self-care measures, such as washing your baby’s scalp daily with a mild shampoo, can help loosen and remove the cradle cap scales. If cradle cap persists or seems severe, your doctor may suggest a medicated shampoo, lotion or other treatment.
Symptoms:-
Common signs of cradle cap include:
*Skin lesions
*Plaques over large area
*Greasy, oily areas of skin
*Skin scales — white and flaking, or yellowish, oily, and adherent — “dandruff”
*Itching — may become more itchy if infected
*Mild redness
*Hair loss
*Patchy scaling or thick crusts on the scalp
*Greasy skin covered with flaky white or yellow scales
*Skin flakes or dandruff
*Possibly mild redness
Similar scales may also be present on the ears, eyelids, nose and groin.
Cradle cap is most common in newborns. It isn’t contagious and probably won’t bother your baby. In most cases, the condition isn’t itchy for infants.
Causes:
Cradle cap is not caused by a bacterial infection, allergy, nor from poor hygiene. Doctors are not in agreement as to the causes, but the two most common hypotheses include fungal infection and overactive sebaceous glands.
In many cases, what is commonly called cradle cap is actually a fungal infection. This infection may be related to antibiotics given to the mother just before the infant’s birth, or the infection could be related to antibiotics routinely given to infants during the first week of life. Antibiotics kill both harmful bacteria as well as the helpful bacteria that prevent the growth of yeast, which is why people who are prone to fungal infections will often discover a fungal infection after taking a round of antibiotics. In infants, the fungus is mostly likely to appear on the scalp (cradle cap), diaper area (fungal diaper rash, jock itch), ear (fungal ear infection, or an ear infection that does not respond to antibiotics),or in the mouth (thrush).
Another common cause of cradle cap appears to be a common manifestation of biotin insufficiency. This may be due, in part, to the influence of biotin on fatty acid biosynthesis. Possibly it has to do with overactive sebaceous glands in the skin of newborn babies, due to the mother’s hormones still in the baby’s circulation. The glands release a greasy substance that makes old skin cells attach to the scalp instead of falling off as they dry. There may be a relationship with skin yeasts (Pityrosporum ovale, newly renamed Malassezia furfur). Seborrheic dermatitis is the adult version of cradle cap
SOME SIGNS OF WARNING:-
If the condition thickens, turns red and irritated, starts spreading, appears on other body parts, or if the baby develops thrush (fungal mouth infection), fungal ear infection (an ear infection that does not respond to antibiotics) or a persistent diaper rash, medical intervention is recommended.
Severe cases of cradle cap, especially with cracked or bleeding skin, can provide a place for bacteria to grow. If the cradle cap is caused by a fungal infection which has worsened significantly over days or weeks to allow bacterial growth (impetigo, most commonly), a combination treatment of antibiotics and antifungals may be necessary. Since it is difficult for a layperson to distinguish the difference between sebaceous gland cradle cap, fungal cradle cap, or either of these combined with a bacterial infection, medical advice should be sought if the condition appears to worsen.
Cradle cap is occasionally linked to immune disorders. If the baby is not thriving and has other problems (e.g. diarrhoea), a doctor should be consulted.
Possible Complications:
•Psychological distress, low self esteem, embarrassment
•Secondary bacterial or fungal infections
Treatment:
Treatment other than gentle washing is not necessary in most mild cases (flaking, with or without small patches of yellow crusting), as the problem often resolves itself whether the cause is sebaceous-gland-related or fungal, but since many patients (and/or parents) are concerned about cosmetic issues, the following options are often considered:
-For all ages: Home remedies include the application of various oils, lotions, or petroleum jelly. There is little adequate or controlled research to support or negate the usefulness of most common home remedies at any age, but there is anecdotal evidence to support either position. When cradle cap is related to fungal infection, treatment for other fungal infections can also work. Tinea capitis is one example of a fungal cause. Doctors may prescribe a seven-day daily application of clotrim (commonly prescribed for jock itch or athlete’s foot) or miconazol nitrate (commonly prescribed for vaginal yeast infections).
-For infants: in cases that are related to fungal infection, doctors may recommend once-daily application of clotrim (1%) or miconozal nitrate (2%) for seven to fourteen days.
-Application of lavender oil may be helpful for fungal infection.
-For toddlers: doctors may recommend a treatment with a mild dandruff shampoo such as Selsun Blue or Neutrogena T-gel, even though the treatment may cause initial additional scalp irritation. A doctor may instead prescribe an antifungal soap such as ketoconazole (2%) shampoo, which can work in a single treatment and shows significantly less irritation than over-the-counter shampoos such as selenium sulfide shampoos, but no adequate and controlled study has been conducted for pediatric use as of 2010.
-For adults: Seborrheic dermatitis (the adult version of cradle cap) usually requires the use of an antifungal shampoo, possibly along with the nightly application of an antifungal cream or an anti-itch cream/gel like Scalpicin. Some doctors also recommend the supplementation of a B-vitamin complex to improve fatty acid metabolism..
Scalp, behind ears, eyebrows:
The common home remedy of applying oil (vegetable, particularly olive oil, or mineral oil) liberally to the scalp and letting it soak in overnight or for lesser periods of time seems to conflict with the fact that Malassezia yeasts thrive in oily environments preferring saturated fats, although anecdotal reports suggest it may be effective. This may be because olive oil is primarily unsaturated fat and does not promote fungal growth. If the cradle cap is not severe, you may try to comb it out gently after bathing. The softened scales can then be brushed away with a soft brush, comb or cloth, but if not done very gently, this can worsen the condition and bring about temporary hair loss. There has been no studies done on these recommendations. Applying petroleum jelly (e.g., Vaseline) liberally overnight is another popular treatment. The softened scales either fall off during the night, or can be brushed off in the morning. Making a paste from sodium bicarbonate (baking soda) and leaving it on the affected area for 10 minutes can also help lift the scales.
[amazon_link asins=’B00EB4OMIM,B00EB4OKVG’ template=’ProductCarousel’ store=’finmeacur-20′ marketplace=’US’ link_id=’94e2006a-2270-11e7-8927-ada705c15d17′]
There is broad disagreement regarding the role of shampoos. Some sources warn against frequent shampooing, others recommend it. Mild baby shampoo is often recommended, while never specifying what “mild” actually means. Baby shampoos often contain detergent surfactants, perfumes, quaternium-15 and other eczemagenic irritants. Again, no studies have been performed on non-prescription shampoos.
Keratolytic (dandruff) shampoos (e.g. with sulfur, selenium, zinc pyrithione, or salicylic acid) are generally not recommended as they sting eyes and may worsen the dermatitis. In stubborn cases some doctors do recommend them while others warn against the use of medicated shampoos in newborns due to systemic absorption. Dandruff shampoos often contain sodium dodecyl sulfate, a noted skin irritant.
Steroid and tar preparations have also been used but have significant drawbacks. Immunomodulators (tacrolimus/Protopic, pimecrolimus/Elidel) have not been approved for babies under two years.
Ketoconazole shampoos and creams are taking first place in medical treatment of moderate to serious cradle cap. Research so far indicates that this anti-fungal medication is not absorbed into the bloodstream. Ketoconazole shampoo is currently made with a number of problematic irritants and allergens.
A Swedish study found good results from massaging the scalp with small amounts of borage oil twice a day.
Other home remedies recommended in various alternative sources and parent forums are herbal washes (e.g. burdock or chamomile), aloe gel, and tea tree oil (Melaleuca oil) shampoo. Tea tree oil and aloe can be sensitizers; any worsening should be an occasion to discontinue the remedy in question. Both remedies have been tested in medical trials and found useful.
Eyelids:…….click & see
Typical medical advice is to use diluted baby shampoo on a cotton swab to cleanse the eyelid. There is no agreement on the dilution, which ranges from a few drops to a half cup warm water, to a 50/50 mix. No studies have been performed on the efficacy or safety of this treatment. (Please note the problems with baby shampoo noted above.) In adults, a study comparing soap and baby shampoo to commercial eyelid scrubs found that patients strongly preferred not to put soap or shampoo on their eyelids. Baking soda has also been recommended (a teaspoonful in a cup of boiled water) and is well accepted by adults. Boiled warm water wash may help.
Prognosis:
As the baby matures this conditions will be cleared.However, studies have shown that the condition occasionally persists into the toddler years, and less commonly into later childhood. It tends to recur in adolescence and persists into adulthood. In an Australian study, about 15 percent of previously diagnosed children still had eczema 10 years later. Sometimes, cradle cap turns into atopic dermatitis. Rarely, it turns out to be misdiagnosed psoriasis.
Prevention:
Shampooing your baby’s hair every few days can help prevent cradle cap. Stick with a mild baby shampoo unless your baby’s doctor recommends something stronger.
The severity of cardle cap can be lessened by controlling the risk factors and by paying careful attention to skin care.
Disclaimer: This information is not meant to be a substitute for professional medical advise or help. It is always best to consult with a Physician about serious health concerns. This information is in no way intended to diagnose or prescribe remedies.This is purely for educational purpose.
Resources:
http://www.bbc.co.uk/health/physical_health/conditions/cradlecap2.shtml
http://www.nlm.nih.gov/medlineplus/ency/article/000963.htm
http://www.mayoclinic.com/health/cradle-cap/DS01074
http://en.wikipedia.org/wiki/Cradle_cap
http://www.livestrong.com/article/294548-itchy-scalp-behind-my-ears/
http://www.dermis.net/dermisroot/en/39521/image.htm
:
Related articles
- How do I cure infant cradle cap? (zocdoc.com)
- Best Products for Getting Rid of Cradle Cap (brighthub.com)
- Cradle Cap, Baby Acne – How to Safely Treat Newborn Skin (pipermartin.wordpress.com)
- What Is Cradle Cap? What Causes Cradle Cap? (medicalnewstoday.com)
- How to Care for the Skin of Your Baby (treatyourskin.wordpress.com)
- Getting to the Root of Scalp Eczema (everydayhealth.com)
- Tips for Baby’s Bath Time (brighthub.com)
- What can I do about a recurring ringworm problem? (zocdoc.com)
- What’s Causing Flaky Patches on the Scalp? (everydayhealth.com)
- People who make mundane tasks fun (behindthezine.wordpress.com)




























![Reblog this post [with Zemanta]](https://i0.wp.com/img.zemanta.com/reblog_e.png?w=580)









