Definition:
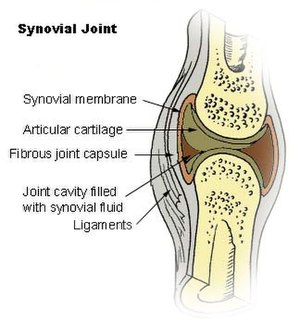
Synovitis is the medical term for inflammation of a synovial membrane, which line those joints which possess cavities, namely synovial joints. The condition is usually painful, particularly when the joint is moved. The joint usually swells due to fluid collection.
It is the inflammation of a synovial (joint-lining) membrane, usually painful, particularly on motion, and characterized by swelling, due to effusion (fluid collection) in a synovial sac.
Description:
Synovitis occurs when the synovium, which lines and lubricates the knee joint, becomes inflamed. The condition can be caused by rheumatoid arthritis or injury/trauma, but sometimes the cause is unknown. The inflammation is caused by fluid collection in response to the injury, which is one of the body’s protection mechanisms….click to see
You may click to see different pictures
CLICK TO SEE THE PICTURES….>...(1)....(2)..…...(3)..….…(4)..….
There are synovial membranes in the hip, knee, wrist, shoulder and ankle joints, and synovitis can occur in any of them, but the knee is most commonly affected. Diseases like arthritis can lead to chronic synovitis, which keeps coming back. Injuries cause acute synovitis, which usually passes if the joint is allowed to rest. If acute synovitis is ignored, however, it can become chronic.
Synovial fluid is a transparent, viscid fluid secreted by the synovial membrane and found in joint cavities, bursae, and tendon sheaths.
Analysis of synovial fluid aspirated from a joint can confirm or rule out various joint diseases such as traumatic arthritis, osteoarthritis, gout, and rheumatoid arthritis.
Synovitis is a risk in several forms of arthritis as well as rheumatoid arthritis, lupus, gout, and other conditions. Synovitis is one part of distinguishing rheumatoid arthritis from other forms of arthritis, although it can be found mildly in osteoarthritis. Long term occurrence of synovitis can result in degeneration of the joint.
Causes :
Synovitis may be due to a metabolic disease such as rheumatoid arthritis, or it may simply be the result of local trauma while running.
Synovitis is a major problem in rheumatoid arthritis, in juvenile arthritis, in lupus, and in psoriatic arthritis. It may also be associated with rheumatic fever, tuberculosis, trauma, or gout.
Rheumatoid arthritis involves synovitis. In rheumatoid arthritis, the synovial membrane lining the joint becomes inflamed. The cells in the membrane divide and grow and inflammatory cells come into the joint from other parts of the body.
Physical Exam Findings
“Joint tenderness is not as reliable or accurate as joint swelling in the assessment of synovitis. Visual inspection alone may be the simplest and most reliable technique for assessing synovitis in rheumatoid arthritis.”
Symptoms:-
Because of the mass of inflammatory cells in rheumatoid arthritis, the joint appears swollen and feels puffy or boggy to the touch. The increased blood flow that is a feature of the inflammation makes the joint warm. The cells release enzymes into the joint space which causes further pain and irritation. If the process continues for years, the enzymes may gradually digest the cartilage and bone of the joint leading to chronic pain and degenerative changes.
The synovium is a thin, filmy material which forms a sac enclosing a freely movable joint in the body. In a healthy joint, it is barely more than one cell thick. It works with cartilage to reduce friction in the knee. There are two types of cells in the synovium. One produces fluid to lubricate the joint, and the other keeps the joint clean by ingesting unwanted materials. When the synovium becomes inflamed, it produces excess fluid, causing the joint to swell.
When injury related (acute), this condition is sometimes called “water on the knee.” If acute synovitis is recognized quickly, rest is usually enough to calm the inflammation. But if left alone, acute synovitis can become chronic. It can also cause adhesions to form on the joint.
In addition to arthritis-related and injury-related synovitis, there are two other common types of the condition:
Toxic, or transient synovitis causes hip pain and limping in children. Its cause is unknown, though it often follows viral infections like chickenpox. It usually disappears as mysteriously as it came and leaves no lasting problems.
Pigmented Villonodular Synovitis (PVNS), which usually occurs in the knee but can be found in other joints as well, is marked by a rust-colored, iron pigment called hemosiderin. PVNS is often missed or misdiagnosed in its early stages, and treatment usually requires surgery.
Symptoms of synovitis include:
*swelling, with fluid collection
*stiffness
*pain
*a “popping” feeling when you move the joint
Diagnosis:-
In addition to the clinical presentation (warm, red, and swollen joints), the diagnosis may be helped by Synovial Fluid Analysis. This is a test that examines the lubricating fluid secreted by synovial membranes. The test is useful in the diagnosis of some types of arthritis (primarily those caused by infection, gout, or pseudogout). This is done by inserting a needle into the knee, injecting numbing medication, and then removing the fluid which has built up. This fluid is then analyzed in the lab.
A test called the patella tap can help with the diagnosis as well. Sometimes minor swelling is masked by the quadriceps muscles in the thighs. The synovial membrane extends above the patella (the kneecap) for more than an inch, so swelling there can be disguised by the muscles that cover it. For the patella tap, a hand grips the thigh immediately above the patella, pressing fluid down under the patella.
The test takes about half an hour and usually is done in a physician’s office or hospital. No special preparations are necessary. The skin over the joint is cleaned with an antiseptic. Usually, a local anesthetic is injected. Using a thin needle, the physician will withdraw a sample of fluid for analysis, including culture of the fluid if infection is a possible diagnosis, and examination for crystals to diagnose gout or pseudogout.
If needed, medication (usually a corticosteroid preparation) can be injected into the joint space through this needle after the specimen is taken.
Treatment:
In most cases, treatment consists of rest, ice, and anti-inflammatory medicines like aspirin or ibuprofen. Compression with an Ace-like bandage and elevation of the knee Is also usually recommended. More severe inflammation may require cortisone injections or synovectomy, surgical removal of the tissue. If the condition has progressed and the knee has been severely damaged, total knee replacement may be necessary.
The excess fluid can be removed without a synovectomy, but this is only a temporary treatment designed to ease discomfort. If the underlying cause is not treated, synovitis will continue and/or recur.
Symptoms of synovitis can be treated by a doctor with anti-inflammatory drugs such as NSAIDs. Specific treatment depends on the determining cause of the synovitis. Specific treatment is based upon both the presumed cause of the synovitis and the particular patient’s response and level of tolerance of any particular medication.
Ckick to see:Advances In the Treatment Of Synovitis
Click to see for Natural & Herbal Treatment of Synovitis.…...(1)...(2)…..(3)….(4)….(5)
Prevention:
None as such, but local trauma can be limited if your muscles and joints are strong and healthy.
Click to learn more about Synovitis
Disclaimer: This information is not meant to be a substitute for professional medical advise or help. It is always best to consult with a Physician about serious health concerns. This information is in no way intended to diagnose or prescribe remedies.This is purely for educational purpose
Resources:-
http://en.wikipedia.org/wiki/Synovitis
http://www.healthscout.com/ency/68/628/main.html
http://members.lycos.co.uk/runninginjuries/Injuries/Knee/synovitis.htm
http://www.knee1.com/care/condition20.cfm/108
Related articles by Zemanta
- What is Synovitis?
- Celebrex: New Horizon in Arthritis Cure
- TMJ Syndrome
- Relief From the Relentless Pain of Rheumatoid Arthritis
- How Can Rheumatoid Arthritis Affect Your Oral Health
- Arthritis Treatment
- Rheumatism
- Types of Arthritis
- What Causes Joint Pain?
- Healthy Joint Pains
- Herbal Home Remedies for Joint Pain
- Beating Arthritis With Diet and Exercise
- Flexibone Capsules – Relief From Joint Pain
- Joint Pain
- Mastering Rheumatoid Arthritis
