Botanical Name: Pastinaca sativa
Family:Apiaceae
Genus:Pastinaca
Species: P. sativa
Kingdom: Plantae
Order:Apiales
Common Name :Parsnip
Habitat : Parsnip is native to Eurasia. It has been used as a vegetable since antiquity and was cultivated by the Romans, although there is some confusion in the literature of the time between parsnips and carrots. It was used as a sweetener before the arrival in Europe of cane sugar. It was introduced into the United States in the nineteenth century.
Description:
Parsnip is a biennial plant with a rosette of roughly hairy leaves that has a pungent odor when crushed. The petioles are grooved and have sheathed bases. The leaves are once- or twice-pinnate with broad, ovate, sometimes lobed leaflets with toothed margins; they grow up to 40 cm (16 in) long. The flower stalk develops in the second year, growing to a height of 40 to 200 cm (20 to 80 in). It is hairy, grooved, hollow (except at the nodes), and sparsely branched. It has a few stalkless, single-lobed leaves measuring 5 to 10 cm (2 to 4 in) long that are arranged in opposite pairs. The yellow flowers are in a loose, compound umbel measuring 10 to 20 cm (4 to 8 in) in diameter. There are 6–25 straight pedicels, each measuring 2–5 cm (1–2 in) that support the umbellets (secondary umbels). The umbels and umbellets usually have no upper or lower bracts. The flowers have tiny sepals or lack them entirely, and measure about 3.5 mm. They consist of five yellow petals that are curled inward, five stamens, and one pistil. The fruits, or schizocarps, are oval and flat, with narrow wings and short, spreading styles. They are colored straw to light brown, and measure 4–8 mm long….click & see
Parsnip is a biennial plant usually grown as an annual. Its long tuberous root has cream-colored skin and flesh and can be left in the ground when mature as it becomes sweeter in flavor after winter frosts. In its first growing season, the plant has a rosette of pinnate, mid-green leaves. If unharvested, it produces its flowering stem, topped by an umbel of small yellow flowers, in its second growing season. By this time the stem is woody and the tuber inedible. The seeds are pale brown, flat and winged.
Parsnips are grown for their fleshy, edible cream-colored taproots. The roots are generally smooth, although lateral roots sometimes form. Most are cylindrical, but some cultivars have a more bulbous shape, which generally tend to be favored by food processors as they are more resistant to breakage. The plant has a apical meristem that produces a rosette of pinnate leaves, each with several pairs of leaflets with toothed margins. The lower leaves have short stems, the upper ones are stemless, and the terminal leaves have three lobes. The highly branched floral stem is hollow and grooved, and can grow to more than 150 cm (60 in) tall.
Cultivation:
The wild parsnip from which the modern cultivated varieties were derived is a plant of dry rough grassland and waste places, particularly on chalk and limestone. Parsnips are biennials but are normally grown as annuals. Sandy and loamy soils are preferable to silt, clay and stony ground as the latter produce short, forked roots.. Parsnip seed significantly deteriorates in viability if stored for long. Seeds are usually planted in early spring, as soon as the ground can be worked to a fine tilth, in the position where the plants are to grow. The growing plants are thinned and kept weed free. Harvesting begins in late fall after the first frost, and continues through winter. The rows can be covered with straw to enable the crop to be lifted during frosty weather. Low soil temperatures cause some of the starches stored in the roots to be converted into sugars, giving them a sweeter taste.
Propagation :
Seed – sow from late winter to late spring in situ. Seed can be slow to germinate, especially from the earlier sowings, it is best to mark the rows by sowing a few radishes with the parsnips. The seed has a short viability, very few will still be viable 15 months after harvesting
Edible Uses:
The parsnip is usually cooked but can also be eaten raw. It is high in vitamins and minerals, especially potassium. It also contains antioxidants and both soluble and insoluble dietary fiber.
Parsnips resemble carrots and can be used in similar ways but they have a sweeter taste, especially when cooked. While parsnips can be eaten raw, they are more commonly served cooked. They can be baked, boiled, pureed, roasted, fried or steamed. When used in stews, soups and casseroles they give a rich flavor. In some cases, the parsnip is boiled and the solid portions are removed from the soup or stew, leaving behind a more subtle flavor than the whole root, and starch to thicken the dish. Roast parsnip is considered an essential part of Christmas dinner in some parts of the English-speaking world and frequently features in the traditional Sunday Roast. Parsnips can also be fried or thinly sliced and made into crisps. Parsnips can be made into a wine that has a taste similar to Madeira.
In Roman times, parsnips were believed to be an aphrodisiac. However, parsnips do not typically feature in modern Italian cooking. Instead, they are fed to pigs, particularly those bred to make Parma ham.
Medicinal Uses:
In traditional Chinese medicine, the root of Chinese parsnip is used as a herbal medicine ingredient.
Poultice; Women’s complaints.
A tea made from the roots has been used in the treatment of women’s complaints. A poultice of the roots has been applied to inflammations and sores. The root contains xanthotoxin, which is used in the treatment of psoriasis and vitiligo. Xanthotoxin is the substance that causes photosensitivity .
Other Uses:
Insecticide; Repellent.
The leaves and roots are used to make an insect spray. Roughly chop the leaves and roots, put them in a basin with enough water to cover, leave them overnight then strain and use as an insecticide against aphids and red spider mite.
Known Hazards:
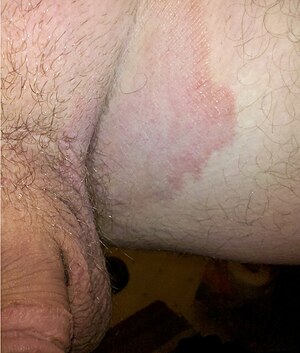
While the root of the parsnip is edible, handling the shoots and leaves of the plant requires caution as the sap is toxic. Like many other members of the family Apiaceae, the parsnip contains furanocoumarin, a photosensitive chemical that causes a condition known as phytophotodermatitis. The condition is a type of chemical burn rather than an allergic reaction, and is similar to the rash caused by poison ivy. Symptoms include redness, burning, and blisters. Afflicted areas can remain discolored for up to two years. Although there have been some reports of gardeners experiencing toxic symptoms after coming into contact with foliage, these have been small in number compared to the number of people that grow the crop. The problem is most likely to occur on a sunny day when gathering foliage or pulling up old plants that have gone to seed. The symptoms have mostly been mild to moderate. The toxic properties of parsnip extracts are resistant to heating, or a storage period of several months. Toxic symptoms can also affect livestock and poultry in parts of their bodies where their skin is exposed. Polyacetylenes can be found in Apiaceae vegetables such as parsnip, and they show cytotoxic activities In sunlight, handling the stems and foliage can cause a skin rash…...click & see
Disclaimer : The information presented herein is intended for educational purposes only. Individual results may vary, and before using any supplement, it is always advisable to consult with your own health care provider.
Resources:
http://en.wikipedia.org/wiki/Parsnip
http://www.pfaf.org/user/plant.aspx?LatinName=Pastinaca+sativa